Health-Related Behaviors of Middle-Aged Cancer Survivors: A Comparative Study with Matched Non-Cancer Controls Using the Korea National Health and Nutrition Examination Survey VI–VII (2013–2018) Data
Article information
Abstract
Background
Middle-aged cancer survivors lack specific health guidelines compared to young and old cancer survivors. Their increased prevalence necessitates the establishment of tailored health guidelines. This study aimed to investigate the health-related behaviors of middle-aged cancer survivors compared to those of the general population.
Methods
This cross-sectional study analyzed 17,332 adults aged 40–65 years who participated in the sixth and seventh Korea National Health and Nutrition Examination Survey (2013–2018). Data on cancer screening, alcohol consumption, smoking, physical activity, sedentary time, and dietary management were collected via self-reported questionnaires. Propensity score matching (1:5) revealed 591 middle-aged cancer survivors and 2,955 non-cancer controls. Descriptive statistics, chi-square tests, and logistic regression analyses were conducted to compare the demographic characteristics and health-related behaviors of both groups.
Results
Multivariate analysis revealed that middle-aged cancer survivors were significantly less likely to consume alcohol (odds ratio [OR]: 0.64; 95% confidence interval [CI]: 0.51–0.81) and smoke (OR: 0.65; 95% CI: 0.43–0.99) and more likely to engage in aerobic physical activity (OR: 1.33; 95% CI: 1.08–1.64) and practice dietary management (OR: 1.47; 95% CI: 1.17–1.84) than the non-cancer controls. However, no significant differences in cancer screening adherence and sedentary time were observed between both groups.
Conclusions
Overall, this study provides fundamental data for the development of tailored health guidelines and patient education programs for cancer survivors.
INTRODUCTION
In addition to the National Cancer Screening Program, various private health screening programs have significantly increased the early cancer detection rate in South Korea [1]. Compared to that in 1999, cancer incidence rate more than doubled in 2019, especially among individuals over 40 years of age [2]. Subsequently, early detection and treatment improved the 5-year survival rate of patients with cancer to 70.7%, leading to a growing population of approximately 2.15 million cancer survivors [2]. Maintaining a healthy lifestyle after primary cancer treatment is crucial to prevent recurrence in cancer survivors. Various lifestyle interventions, such as regular physical activity and dietary modifications, improve the life quality of cancer survivors [3,4]. Prevention of secondary cancer and chronic diseases is necessary to reduce the mortality rate, further emphasizing the importance of lifestyle management, including regular health screening, smoking cessation, moderate alcohol consumption, aerobic exercise, and balanced diet [5,6].
Compared to the young and old cancer survivors, middle-aged cancer survivors face unique challenges in resuming their daily lives after treatment. Many return to work and shoulder family responsibilities while managing the long-term complications of cancer treatment, such as pain, fatigue, and depression. These survivors exhibit a higher risk of developing secondary cancers and chronic diseases than the general population, making good health-related behaviors critical to ensure long-term survival [7]. However, comprehensive health management guidelines specific to middle-aged cancer survivors are limited, with existing recommendations often generalized for all patients with cancer regardless of age [8,9]. Furthermore, long-standing lifestyle habits are difficult to change following cancer diagnosis and adherence to recommended health-related behaviors is often suboptimal in patients with cancer [10]. Therefore, we analyze health-related behaviors that could be recommended to middle-aged cancer survivors, which have not been addressed in previous studies.
This study aimed to assess the health-related behaviors of middle-aged cancer survivors in South Korea using the Korea National Health and Nutrition Examination Survey (KNHANES) data. By comparing their health-related behaviors with those of non-cancer controls, this study provides fundamental data for the development of tailored health guidelines and patient education programs for cancer survivors.
METHODS
Study design and participants
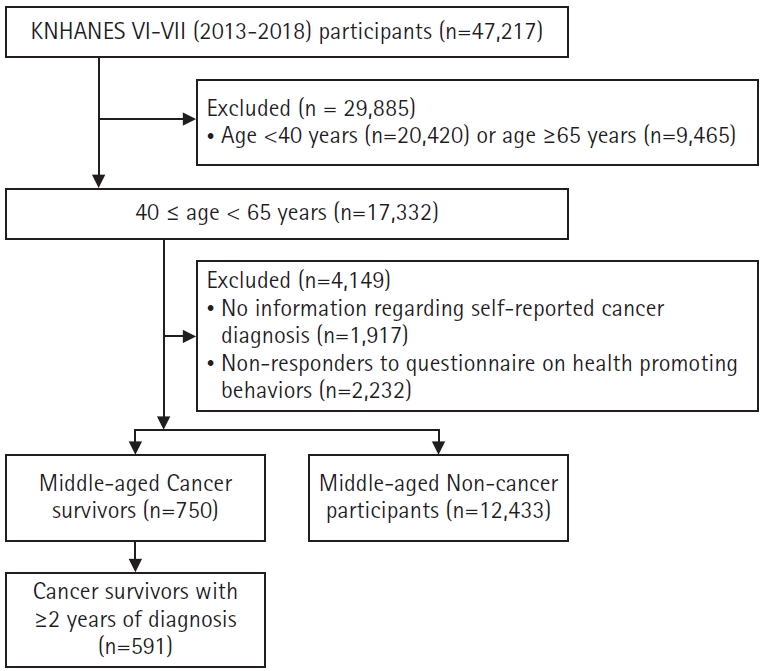
This retrospective study used secondary data from KNHANES to compare the health-related behaviors of middle-aged cancer survivors and non-cancer controls. This study was approved by the Institutional Review Board (IRB) of the Hwasun Chonnam National University Hospital (IRB No. CNUHH-2022-108). The dataset was officially approved as national statistics (approval No. 117002) and collected according to the National Health Promotion, Statistics, and Personal Information Protection Acts. KNHANES VI (2013–2015) and VII (2016–2018) data were analyzed. Out of 47,217 survey participants, only 17,332 individuals aged 40–65 years were included in this study. Participants who answered “don’t know” or refused to answer the questions related to cancer diagnosis (n=1,917) and health-related behaviors (n=2,232) were excluded from the study, resulting in a final sample size of 13,183 individuals. Among these individuals, only 750 had a history of cancer, with 12,433 individuals having no cancer history. To maintain a homogenous sample, individuals diagnosed within the past 2 years were excluded due to ongoing acute treatment and post-treatment effects, such as emotional stress, anxiety, depression, fatigue, and physical impairments [11]. Consequently, the final sample included 591 middle-aged cancer survivors diagnosed within the last 2 years (Fig. 1).
Variables
Study variables included sociodemographic characteristics, such as age, sex, marital status, education level, employment status, household income, and residential area, body mass index (BMI), comorbidities, activity limitations, stress level, and self-reported health status. According to the criteria established by the Korean Society for the Study of Obesity, the participants were categorized as underweight (<18.5 kg/m2), normal weight (18.5–24.9 kg/m2), or obese (≥25.0 kg/m2) based on their BMI [12]. The participants were further categorized as married or non-married (single, divorced, or separated) based on their marital status and as <high school, high school graduate, or ≥college graduate based on their education level. Additionally, the participants were classified as employed or unemployed based on their employment status and categorized into four groups (low, middle-low, middle-high, and high income) based on their household income. Based on their residential area, they were categorized as urban or rural. Comorbidities included physician-diagnosed conditions, such as hypertension, dyslipidemia, cardiovascular diseases, arthritis, chronic respiratory diseases, diabetes, thyroid diseases, depression, chronic kidney disease, and liver diseases (hepatitis B, hepatitis C, and cirrhosis). Activity limitations were assessed with the question, “Do you have any limitations in your daily life and social activities due to current health problems or physical/mental disabilities?” The responses were categorized as “Yes” or “No.” Stress level was assessed with the question, “How much stress do you usually experience in daily life?” The responses were categorized as none, mild, moderate, or severe. Self-reported health status was assessed with the question, “How would you rate your overall health?” The responses were categorized as good, fair, or poor.
Health-related behaviors
Health-related behaviors were assessed based on the key lifestyle factors associated with cancer prevention and survival. Cancer screening adherence was defined as having undergone screening within the past 2 years, including both self-paid screening at comprehensive health centers and that provided by the National Health Insurance Corporation. Participant responses for screening adherence were categorized as “Yes” or “No.” Alcohol consumption was assessed based on the “monthly drinking rate” indicated in the KNHANES data, with participant responses classified as “Yes” if they consumed alcohol at least once per month or “No” if they were lifetime abstainers or consumed alcohol less than once per month. Based on their smoking status, the participants were classified as “current smokers” or “non-smokers/former smokers who quit smoking.” Physical activity was assessed according to the World Health Organization guidelines, with moderate-intensity activity defined as at least 150 minutes activity per week, vigorous-intensity activity as at least 75 minutes activity per week, or equivalent combination of both moderate and vigorous activities (1 minute of vigorous activity=2 minutes of moderate activity) [13]. Sedentary time was evaluated based on the self-reported daily sitting time, with prolonged sedentary time (>7 hr/day) classified as a risk factor for increased mortality [14]. Patient responses to the dietary control question, “Do you control your diet for special health reasons?” were categorized as “Yes” or “No.”
Statistical analyses
As the KNHANES data were collected using a complex sampling design rather than complete enumeration, survey weights, stratification variables, and cluster variables were incorporated into the statistical analyses. For the sociodemographic characteristics, unweighted numbers and weighted percentages were used as categorical variables, whereas means and standard errors were used as continuous variables.
Propensity score matching (PSM) was performed using a non-random package in R, version 4.1.0 to minimize the selection bias [15]. Each middle-aged cancer survivor was matched with five non-cancer controls based on variables potentially influencing the health-related behaviors, including age, sex, BMI, marital status, education level, employment status, household income, residential area, comorbidities, activity limitations, stress level, and self-reported health status. Univariate analyses were conducted using chi-square tests, whereas multivariate analyses were performed using binary logistic regression. Multivariate logistic regression models were developed using two approaches to evaluate the health-related behaviors before and after PSM. Model 1 was adjusted for PSM and significant variables (P<0.1) identified via the univariate analyses of health-related behaviors, whereas Model 2 was adjusted for PSM and all covariates. Two-tailed P-value <0.05 was considered statistically significant. All statistical analyses, except PSM, were performed using SPSS ver. 28.0 (IBM Corp.).
RESULTS
Patient characteristics before and after propensity score matching
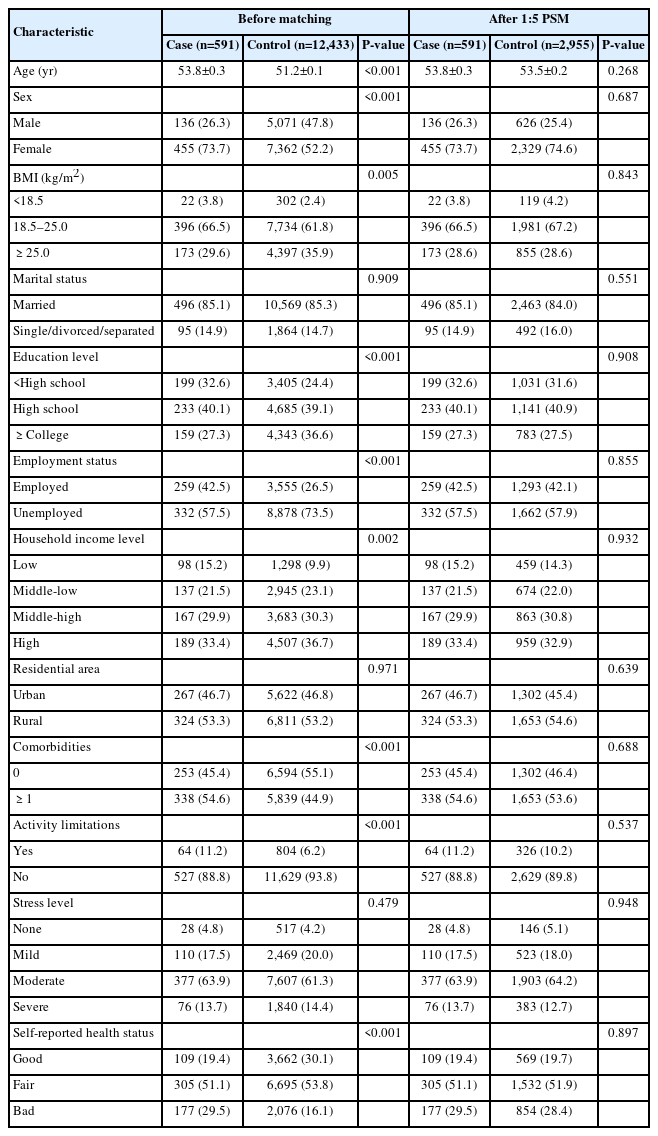
Patient characteristics before and after PSM are presented in Table 1. Among the 13,024 participants, mean age of the 591 cancer survivors, including 136 males (26.3%) and 455 females (73.7%), was 53.8 years. Before matching, mean age of 12,433 non-cancer participants, including 5,071 males (47.8%) and 7,362 females (52.2%), was 51.2 years. After 1:5 PSM, the final sample comprised 591 cancer survivors and 2,955 non-cancer controls. Prior to matching, significant differences in baseline characteristics, including age, sex, BMI, education level, employment status, household income, comorbidities, activity limitations, and self-reported health status, were observed between both groups (P<0.05). However, after matching, no significant difference in any characteristic was observed between both groups (P>0.05), confirming successful matching.
Cancer types
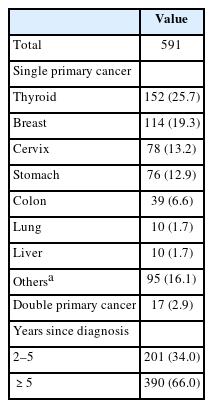
Among the 591 middle-aged cancer survivors, thyroid cancer (n=152; 25.7%) was the most common, followed by breast (n=114; 19.3%), other (n=95; 16.1%), cervical (n=78; 13.2%), stomach (n=76, 12.9%), colon (n=39; 6.6%), liver (n=10; 1.7%), and lung (n=10; 1.7%) cancers. Notably, 17 participants (2.9%) were diagnosed with multiple primary cancers. The time elapsed since diagnosis was ≥2 years but <5 years in 201 participants (34.0%) and ≥5 years in 390 participants (66.0%) (Table 2).
Comparison of health-related behaviors before and after propensity score matching
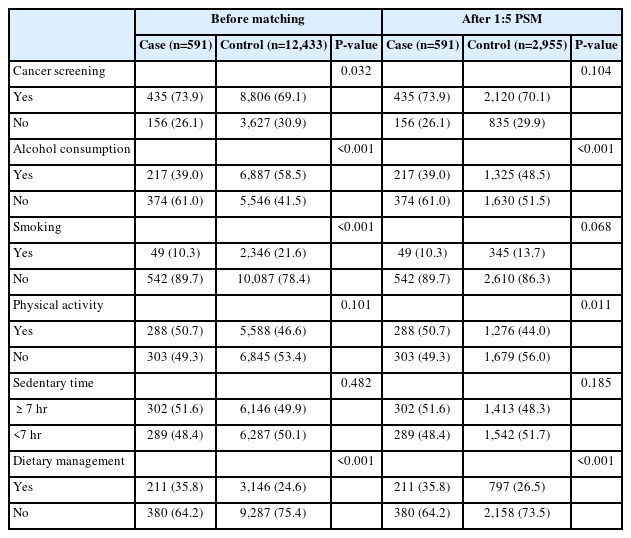
Health-related behaviors of both groups before and after PSM are presented in Table 3. After matching, significant differences in alcohol consumption, physical activity, and diet were observed between both groups. In total, 217 middle-aged cancer survivors (39.0%) consumed alcohol compared to the 1,325 controls (48.5%) (P<0.001). Moreover, 288 cancer survivors (50.7%) engaged in moderate or vigorous physical activity, and 1,276 controls (44.0%) adhered to the recommended physical activity guidelines (P=0.011). Dietary management was significantly different between both groups, with only 211 cancer survivors (35.8%) showing diet adherence compared to the 797 controls (26.5%) (P<0.001). However, no significant differences in cancer screening adherence, smoking status, and sedentary time were noted between both groups.
Logistic regression analysis of health-related behaviors
Next, multivariate logistic regression analyses were conducted to examine the differences in health-related behaviors between middle-aged cancer survivors and non-cancer controls (Table 4). In Model 1, which was adjusted for PSM and significant covariates (P<0.1) determined via univariate analyses, middle-aged cancer survivors were significantly less likely to consume alcohol (odds ratio [OR]: 0.64; 95% confidence interval [CI]: 0.51–0.81) and smoke (OR: 0.64; 95% CI: 0.42–0.97) but more likely to engage in physical activity (OR: 1.33; 95% CI: 1.08–1.63) and practice dietary management (OR: 1.47; 95% CI: 1.17–1.83) than the non-cancer controls. No significant differences in cancer screening adherence and sedentary time were observed between both groups.
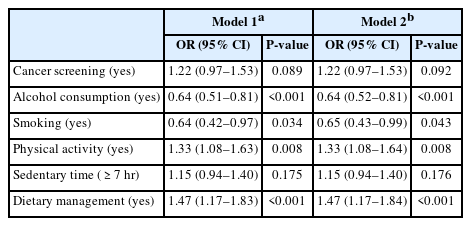
Multivariate analyses of the health-related behaviors of the cancer survivors and non-cancer controls
Model 2, which was adjusted for PSM and all covariates, showed the same results, with middle-aged cancer survivors exhibiting lower odds of alcohol consumption (OR: 0.64; 95% CI: 0.52–0.81) and smoking (OR: 0.65; 95% CI: 0.43–0.99) and higher odds of engaging in physical activity (OR: 1.33; 95% CI: 1.08–1.64) and practicing dietary management (OR: 1.47; 95% CI: 1.17–1.84) than the non-cancer controls. However, no significant differences in cancer screening adherence and sedentary time were noted between both groups. All logistic regression models incorporated sampling weights to account for the complex survey design of KNHANES.
DISCUSSION
This study investigated the differences in the health-promoting behaviors of middle-aged cancer survivors and non-cancer participants. Notably, cancer survivors exhibited lower odds of alcohol consumption and smoking and higher odds of aerobic physical activity and diet adherence than the non-cancer controls. However, no significant differences in cancer screening adherence and sedentary time were observed between both groups.
Owing to the increasing number of cancer survivors, secondary cancer prevention has become a major public health concern [16]. Various risk factors, including smoking, alcohol consumption, poor nutrition, and physical inactivity, contribute to primary and secondary cancer development [17]. Specifically, middle-aged cancer survivors are more vulnerable to cardiovascular comorbidities, such as hypertension, obesity, and smoking-related diseases, than the old cancer survivors [18]. Therefore, adopting and maintaining good health-related behaviors are essential to improve the long-term health outcomes and sustain functional independence in middle-aged cancer survivors.
Continuous smoking and alcohol consumption even after cancer diagnosis are strongly associated with the increased risk of chronic diseases and metabolic syndrome [19,20] and high likelihood of cancer recurrence and development of secondary malignancies [21,22]. Therefore, healthcare professionals emphasize the importance of smoking cessation and reduced alcohol consumption to prolong the survival of middle-aged cancer survivors. In this study, cancer survivors exhibited lower odds of smoking and alcohol consumption than the non-cancer controls, consistent with previous reports [23-25]. Dietary habits and physical activity play crucial roles in addressing nutritional deficiencies, preserving the muscle mass, and managing metabolic imbalances after cancer treatment [26]. Consumption of a nutritionally balanced diet is associated with a low mortality risk in cancer survivors [27]. Cancer survivors in their 50s have greater awareness of food safety than those in other age groups [28]. Although this study did not assess the specific dietary patterns, middle-aged cancer survivors showed dietary adherence more consistently than the controls. Regular aerobic physical activity is associated with improved physical function, reduced psychological distress, and enhanced overall quality of life [29]. In this study, middle-aged cancer survivors engaged in physical activity more than the controls. These reports highlight the need for structured guidelines focusing on minimizing the risk of exercise-related injuries to ensure the safe and effective implementation of exercise programs for cancer survivors.
Secondary primary cancer, which is distinct from cancer recurrence and metastasis, is a newly diagnosed malignancy in individuals with cancer history. Cancer survivors exhibit a significantly higher risk of secondary cancer development than the general population [5]. Despite this increased risk, many survivors do not undergo the recommended secondary cancer screening, often due to limited awareness and healthcare access [30,31]. A previous study reported higher cancer screening adherence in middle-aged cancer survivors than in the general population due to improved information dissemination [7]. In contrast, this study revealed no significant difference in cancer screening adherence between the middle-aged cancer survivors and non-cancer controls. This suggests that external factors, such as healthcare accessibility, insurance coverage, and socioeconomic barriers, influence cancer screening adherence more than individual awareness. Future studies should explore these determinants to facilitate the establishment of targeted interventions to promote cancer screening. Moreover, considering the lack of standardized secondary cancer screening guidelines, healthcare providers should emphasize the importance of routine screening to facilitate the early detection and timely treatment of patients.
Sedentary behaviors, defined as activities requiring energy expenditure <1.5 metabolic equivalents while sitting, reclining, or lying down, are growing health concerns for cancer survivors [32]. Prolonged sedentary time >10 hr/day is associated with increased all-cause mortality and reduced quality of life in cancer survivors [33-35]. Therefore, the World Health Organization [36] recommends engaging in physical activities of any intensity in sedentary time. Simple behavioral modifications, such as using stairs instead of elevators, engaging in brief high-intensity exercises, and minimizing screen time, reduce the sedentary time and improve the overall health of individuals. Notably, this study indicated no significant difference in sedentary time between the middle-aged cancer survivors and non-cancer controls, possibly due to its greater focus on engaging in moderate–vigorous physical activity than on specific efforts to reduce sedentary time. Therefore, future studies should investigate whether reducing sedentary time independent of physical activity levels improves the long-term health outcomes of cancer survivors. Moreover, use of wearable technology with real-time activity tracking can provide objective data on sedentary time and its impact on cancer survival.
This study has several strengths. Use of a large nationally representative dataset and PSM reduced the selection bias, thereby improving the reliability of the findings. Unlike previous studies that grouped different age ranges and cancer types, this study specifically focused on the middle-aged cancer survivors, thereby providing specific insights into this population. As middle-aged individuals are actively engaged in the workforce and often serve as caregivers, good health-related behaviors are particularly important for their long-term well-being. Furthermore, this study highlights the importance of reducing the sedentary time and increasing the physical activity of cancer survivors. Although no significant difference in sedentary time was observed between the middle-aged cancer survivors and non-cancer controls, targeted interventions are necessary to change the sedentary behaviors of middle-aged cancer survivors.
This study has some limitations. First, cancer stage was not considered, which may have influenced the findings, as individuals with advanced cancer often exhibit physical limitations affecting their activity levels. Therefore, future studies should assess cancer staging to provide more comprehensive insights. Second, self-reported nature of the survey may have introduced potential recall bias and subjective variability, particularly in dietary and physical activity assessments. Third, this cross-sectional study did not determine the associations between cancer survival and health-related behaviors, warranting further longitudinal studies. Nevertheless, this study provided valuable insights into the health-related behaviors of middle-aged cancer survivors, facilitating the development of tailored interventions to enhance their long-term survival.
In conclusion, although middle-aged cancer survivors exhibited health-promoting behaviors, including reduced alcohol consumption and smoking, high physical activity, and dietary adherence, some gaps persisted in their preventive care. This study highlights the importance of secondary cancer screening and reduced sedentary time for the enhanced survival of these individuals. Furthermore, targeted interventions are necessary to address the existing gaps and improve the long-term health outcomes of middle-aged cancer survivors.
Notes
AUTHOR CONTRIBUTIONS
Dr. Yu Ri CHOE ad full access to all of the data in the study and takes responsibility for the integrity of the data and the accuracy of the data analysis. All authors reviewed this manuscript and agreed to individual contributions.
Conceptualization: all authors. Data curation: MLK and JRJ. Formal analysis: JRJ and YRC. Investigation: MLK. Methodology: MLK and JRJ. Project administration: MLK and YRC. Software: JRJ and YRC. Supervision: YRC. Validation: YRC. Visualization: JRJ and YRC. Writing–original draft: MLK. Writing–review & editing: JRJ and YRC.
CONFLICTS OF INTEREST
No existing or potential conflict of interest relevant to this article was reported.
FUNDING
None.
DATA AVAILABILITY
The data presented in this study are available upon reasonable request from the corresponding author.