| Korean J Health Promot > Volume 25(1); 2025 > Article |
|
ABSTRACT
Background
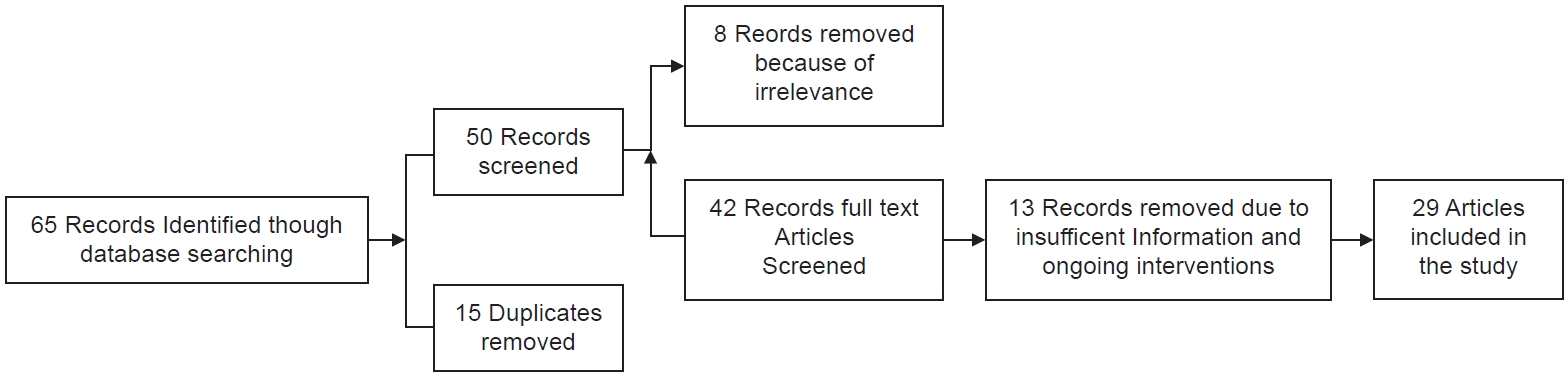
Methods
Results
Conclusions
AUTHOR CONTRIBUTIONS
Dr. Melika Geleta DESALEGN had full access to all of the data in the study and takes responsibility for the integrity of the data and the accuracy of the data analysis. All authors reviewed this manuscript and agreed to individual contributions.
Conceptualization: all authors. Data curation: all authors. Writing–original draft: all authors. Writing–review & editing: all authors.
CONFLICTS OF INTEREST
No existing or potential conflict of interest relevant to this article was reported.
FUNDING
This study was supported by the Korea International Cooperation Agency (KOICA) (No. P2019-00160-1).
Table 1.
| First author | Year | Study design | Study participants | Types of intervention | Main findings |
|---|---|---|---|---|---|
| Dennis [1] | 2017 | Systematic review | Women in LMICs | Antenatal & postnatal depression | High prevalence of antenatal and postnatal depression in LMICs |
| Tol [2] | 2020 | Systematic review & meta-analysis | LMIC populations | Maternal mental health interventions | Positive impact on child-related outcomes |
| Giebel [3] | 2024 | Review | LMIC populations | Community-based mental health interventions | Key lessons for program development |
| Assefa [4] | 2019 | Review | General population in Ethiopia | Community health extension program | Successes and challenges in primary health care |
| Hailemariam [5] | 2019 | Systematic review | Ethiopia | Mental health integration into primary care | Effective implementation strategies identified |
| Yaya [6] | 2018 | Multilevel analysis | Mothers in South Africa | Maternal healthcare service utilization | Individual & community factors influencing service use |
| Berhanu [7] | 2017 | Cluster-randomized trial | Rural Ethiopian women | Community-based maternal care package | Increased health facility use, reduced stillbirth rate |
| Dadi [8] | 2020 | Umbrella review | Global antenatal population | Antenatal depression | Association with adverse birth outcomes |
| Fekadu [9] | 2016 | Mixed methods | Rural Ethiopia | Scalable mental healthcare plan | Development of an intervention framework |
| Hanlon [10] | 2010 | Cross-sectional | Ethiopian postpartum women | Sociocultural practices & mental health | Association with postnatal common mental disorders |
| Rahman [11] | 2013 | Systematic review & meta-analysis | LMIC perinatal women | Common perinatal mental disorder interventions | Effective in reducing symptoms |
| Tenaw [12] | 2024 | Systematic review & meta-analysis | Teenage mothers | Psycho-social interventions for postpartum depression | Effective in prevention |
| Jackson [13] | 2016 | Cross-sectional | Pregnant women in rural Ethiopia | Role of health extension workers | Facilitated health facility linkage for delivery |
| Fekadu [14] | 2015 | Cohort study | Rural Ethiopian population | Mental illness & mortality risk | Higher mortality in severe mental illness cases |
| Hanlon [15] | 2016 | RCT | Ethiopia | Task-sharing for severe mental disorders | Non-inferior outcomes to specialist care |
| Karim [16] | 2018 | Dose-response study | Ethiopian communities | Community-based data for decision-making | Improved maternal & newborn health practices |
| Addisu [17] | 2022 | Systematic review & meta-analysis | Ethiopian women | Maternal health care utilization | Identified barriers and facilitators |
| Liberati [18] | 2009 | Guidline | PRISMA statement for reporting systematic reviews and meta-analyses of studies that evaluate health care interventions: explanation and elaboration | ||
| Higgins [19] | 2019 | Chapter 8 | Systematic reviews | Cochrane handbook for systematic reviews of interventions. 2nd ed. John Wiley & Sons; 2019. p. 205-28 | Assessed the quality of studies included. |
| Tadesse [20] | 2023 | Systematic review protocol | Ethiopia | Maternal morbidity & mortality framework | Proposed intervention strategies |
| Tomlinson [21] | 2018 | Cluster RCT | South Africa | Home visiting by community health workers | Reduced antenatal depression, improved child outcomes |
| Tesfaye [22] | 2010 | Validation study | Ethiopian postpartum women | Screening for postnatal depression | Validated EPDS & Kessler scales |
| Surkan [23] | 2011 | Systematic review & meta-analysis | Developing countries | Maternal depression & child growth | Depression negatively impacts child growth |
| Rtbey [24] | 2024 | Systematic review & meta-analysis | Ethiopian women | Perinatal depression & risk factors | High prevalence & associated factors |
| Ayen [25] | 2024 | Systematic review & meta-analysis | Ethiopian pregnant women | Depression during pregnancy | Key risk factors identified |
| Bitew [26] | 2020 | Qualitative study | Rural Ethiopia | Psycho-social interventions for antenatal depression | Stakeholder perspectives on intervention feasibility |
| Ahmed [27] | 2022 | Systematic review | LMICs | Role of community health workers | Improved health equity outcomes |
| Scroggins [28] | 2024 | Systematic review | Perinatal women | Community-based perinatal mental health interventions | Effective approaches identified |
| Zenebe [29] | 2023 | A cluster-randomized control trial | Southern Ethiopian community | Data for decision-making intervention on maternal and newborn health care practices in Ethiopia | Stakeholder perspectives on intervention feasibility |
REFERENCES
-
METRICS

-
- 1 Crossref
- 0 Scopus
- 2,306 View
- 31 Download
- ORCID iDs
-
Melika Geleta DESALEGN

https://orcid.org/0009-0009-1888-0484EunWoo NAM

https://orcid.org/0000-0002-3517-6247 - Related articles



 PDF Links
PDF Links PubReader
PubReader ePub Link
ePub Link Full text via DOI
Full text via DOI Download Citation
Download Citation Print
Print